Things that can go wrong with non-contact tonometry
Non-contact tonometry is popular in community optometric practice because it can be delegated to a clinical assistant, be conducted as part of a pre-screen (along with auto-refraction) before the person sees the optometrist, doesn’t involve the instillation of uncomfortable anaesthetics, reduces the chance of cross-infection from one patient to another and because in some parts of the world optometrists are not licensed to use any diagnostic drugs.
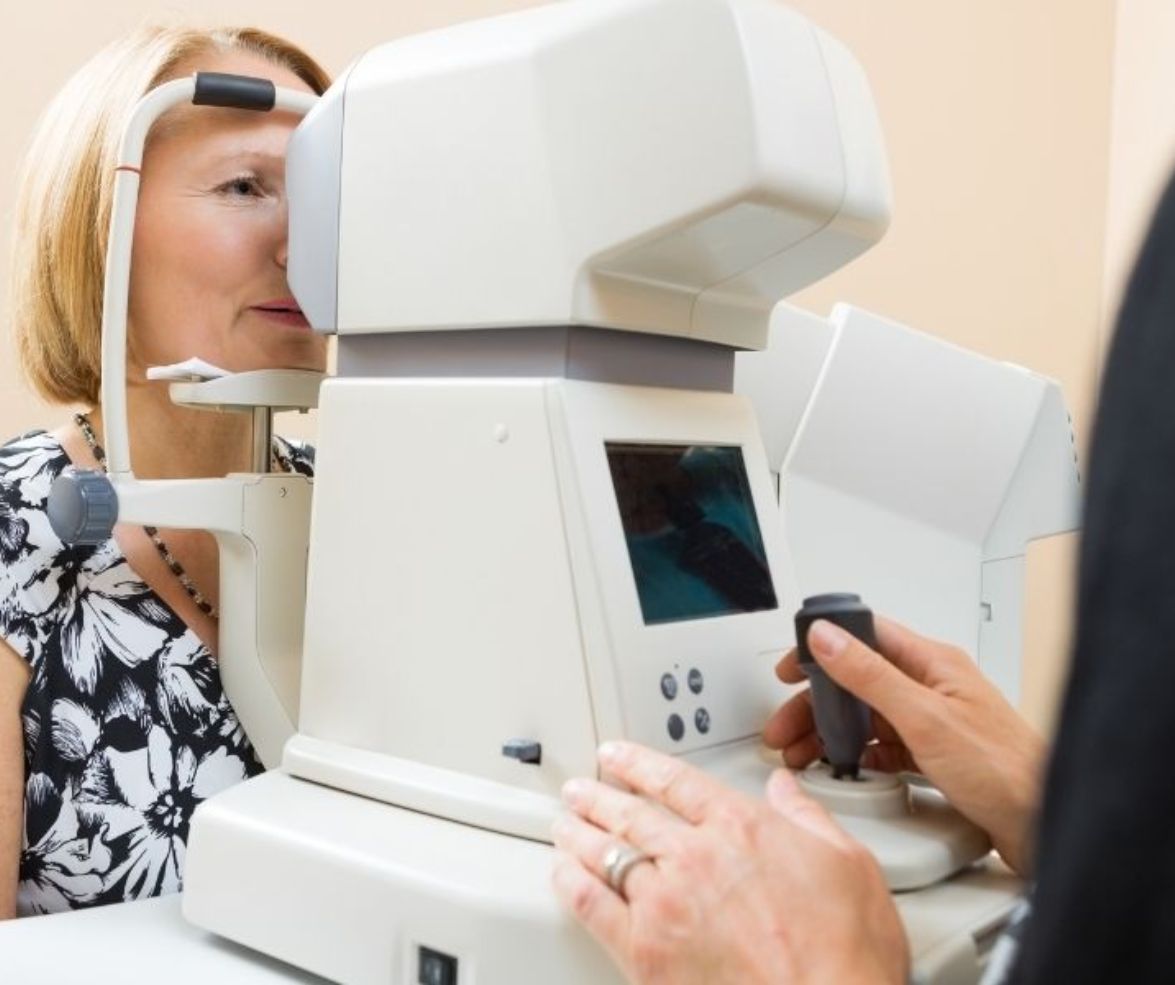
Non-contact tonometers are often located outside of the consulting room so the optometrist can be examining a patient while a clinical assistant is pre-screening the next. This helps with patient flow and practice financial sustainability. Non-contact tonometers are sometimes referred to as the ‘air puff test’ by staff and as ‘the puffer’ by patients. I have never met a patient that looked forward to having the air puff test!


Typical non-contact tonometer set-up A screen on the operator’s side of a
modern non-contact tonometer


Corneal alignment screen The operator’s control panel on a modern
non-contact tonometer
There are several different non-contact tonometers. Some are fully manual where the operator has to position the patient, align the air nozzle with the eye and press a button to take a reading. Others are semi-automated where once alignment has been achieved by the operator, the device will automatically activate the air puff. Others are fully automated where the person rests their head against the head rest (often there is no chin rest-one less thing to keep clean), the machine will automatically align the air nozzle and automatically take three (or more) readings, display the average on the screen and automatically repeat the process for the other eye.
A quick reminder of how non-contact tonometers work. Non-contact tonometers measure intraocular pressure by analysing the cornea's response to a precise, rapid puff of air. Intraocular pressure is calculated based on the time required for the air pulse to flatten the cornea, providing a quick, painless and sterile screening. An infrared light beam (OCT on very modern non-contact tonometers) detects the exact moment the cornea becomes flattened and the instrument measures the force/time required to achieve this. One of the features of the measurement process is the noise the air puff makes when it’s activated. Modern devices use a quiet and gentle air puff which is less likely to make the person blink, jump and be anxious for subsequent measurements.

The principles of non-contact tonometry
The reason that three or more readings are needed per eye are because non-contact tonometers take a reading in a fraction of a second and intraocular pressure changes slightly throughout the heartbeat. Averaging three readings mitigates this, ensuring the result is not biased by a reading taken at an extreme point in the pulse cycle. This is called minimising pulse cycle variability. The intraocular pressure pulse can be seen during Goldmann contact tonometry as the mires pulse slightly. The end point reading is taken when the pressure applied by the operator to the Goldmann probe causes the pulse of the inner edge of the mires to move an equal amount either side of the mid-point. This is why one good intraocular pressure reading with a Goldmann tonometer is sufficient. This is much more difficult to explain in writing than to see in real life.

End point for Goldmann applanation tonometry
In my experience, the operator will struggle to obtain accurate readings in one patient out of twenty. I’ve described the reasons for this below, along with suggestions as to how accurate readings can be obtained despite these problems.
What can go wrong?
Patient characteristics
By patient characteristics I mean things such as blinking just as the air puff is activated, head held back from the head rest, face held at an angle to the air nozzle, unable to get head and/or body into the correct position because of postural or understanding problems. I have seen this happen even with experienced operators. My suggestion is that, before the patient or the operator get frustrated, to ask the person to come back in the next day or two to try again perhaps with a different operator. If this doesn’t work see below in What to do?. Even when the cause of not being able to take a reading is due to patient characteristics the patient should not be blamed. It is never the patient’s fault.
Operator characteristics
By operator characteristics I mean the operator not knowing what to do because of a lack of training and/or experience. A more experienced operator should take over. The novice operator should be given more training to include the reason that three (or more) readings are required, the reason why another reading is required for readings such as 25, 18, 17 and the meaning of any error codes displayed on the screen. Optometrists can be misled if the operator blames patient characteristics for an inability to take readings when the reason is because of operator or tonometer (see below) characteristics. In my experience, under the circumstances of challenging patient characteristics, an experienced operator can always obtain meaningful readings.
Tonometer characteristics
By tonometer characteristics I mean instrument malfunction. It is mandatory for non-contact tonometers to undergo an annual service by a skilled engineer including a calibration check and for service records to be kept in the practice. If the instrument is broken a note should be made in the patient’s clinical records, and an appointment made for a separate intraocular pressure check for after the instrument has been repaired. If the patient fails to attend for the intraocular pressure check they should be texted/phoned/written to (all attempts documented in the clinical records) with an explanation as to the importance of an intraocular pressure check and the possible visual consequences if it is not conducted. The responsibility to get the patient back to the practice is with the optometrist.
If the instrument is fully automatic (automatically lines up the air puff nozzle with the cornea and automatically takes the readings) but won’t take a reading, disengage the automatic feature and use the device manually.
Also, some non-contact tonometers won’t take readings when the intraocular pressure is very high (above 40-varies from instrument to instrument) so an inability to take readings, when patient and operator characteristics are good, could be because the intraocular pressure is very high.
Eye characteristics
By eye characteristics I mean conditions such as dry eye and corneal irregularity such as scarring; anything that interferes with the smoothness of the anterior corneal surface. An irregular corneal surface due to dry eye can be smoothed with the use of artificial tear drops (daily three or four times) and the patient rebooked for an intraocular pressure check in a weeks’ time. Surface irregularities due to corneal scarring can’t be easily fixed and are best dealt with using another type of tonometer-see What to do? below.
What to do?
If readings can’t be obtained, the operator should explain to the optometrist if it is due to patient characteristics, usually blinking or narrowing the palpebral aperture, an error reading (indicated on the tonometer screen) or that readings can’t be obtained even though the patient is cooperative and the operator is experienced. If the latter the optometrist can then determine what to do next by checking for corneal anterior surface irregularities and considering the possibility of very high intraocular pressures.
If there is a high cup-to-disc ratio or it has increased since the last examination and intraocular pressures can’t be obtained using a non-contact tonometer then high intraocular pressures should be suspected and the person referred to an ophthalmologist for further investigation.
If the practice is equipped with another type of tonometer such as iCare rebound or Goldmann applanation then this should be used. If the practice doesn’t have another type of tonometer (this is typically not mandatory) then the person should be advised to attend a practice that does have one. This may be a community practice or a hospital eye department.
There is a thought that when it is difficult to measure intraocular pressures using a non-contact tonometer, to abandon further attempts and to ask the person to undergo visual fields testing instead. The reasoning being that if the visual fields are normal then the intraocular pressure must also be in the normal range and failure to obtain readings is not clinically relevant. However, this is not to be recommended since research has shown that retinal nerve fibre damage due to high intraocular pressure can take many months to appear as a visual field defect. Waiting for a visual field defect to appear before starting treatment causes an unnecessary delay in treatment. If in doubt, don’t faff about!

.jpg)
.jpg)
2.jpg)
2.jpg)

.jpg)
.jpg)
.jpg)
.jpg)


1.jpg)



.jpg)
.jpg)



_(Instagram_Post).jpg)
.jpg)
_(1080_x_1080_px).jpg)


with_UP_Cabinet_Minister_Sh_Nand_Gopal_Gupta_at_OpticsFair_demonstrating_Refraction.jpg)
with_UP_Cabinet_Minister_Sh_Nand_Gopal_Gupta_at_OpticsFair_demonstrating_Refraction_(1).jpg)

.jpg)








.jpg)



.png)




